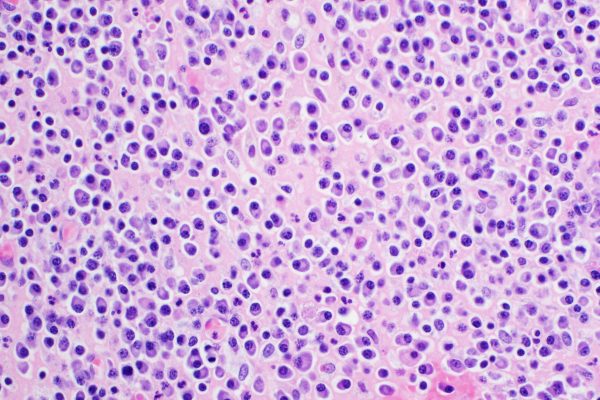
Monoclonal gammopathy of undetermined significance and smouldering multiple myeloma are conditions that precede multiple myeloma. Using time-varying biomarkers, the PANGEA project developed a risk prediction model for patients with these precursor conditions. This approach addresses the limitations of current criteria and improves the ability to predict the risk of progression to multiple myeloma. The results from this study were recently published in The Lancet Hematology.
Multiple myeloma (MM) is often preceded by two precursor conditions, monoclonal gammopathy of undetermined significance (GHUS) and smouldering multiple myeloma (SMM). Currently, various criteria are being used to stratify these patients into risk groups, based on the predicted probability of progression to MM. However, these methods use laboratory measurements at diagnosis and patients are rarely re-stratified according to evolving laboratory findings. As such, there is a need for a prediction model that incorporates time-varying biomarkers that allow to update the risk at later time points. To address this need, the Precursor Asymptomatic Neoplasms by Group Effort Analysis (PANGEA) project developed a MGUS and SMM stratification algorithm that utilised accessible, time-varying biomarkers to model risk of progression to MM.
This retrospective, multicohort study included 6,441 adult patients (≥18 years) with precursor disease to MM with serial laboratory measurements. It involved three different cohorts with patients belonging to different clinical centres: training (Dana-Farber Cancer institute in Boston), validation cohort 1 (University of Athens) and validation cohort 2 (University College London). Two PANGEA models were developed, one including biomarkers that require a bone marrow biopsy (BM), and one excluding these biomarkers (no BM). Both models were designed as multivariate Cox regressions with time-varying biomarkers, built by selecting clinically significant predictors of progression identified in the training cohort and validated in the two validation cohorts. The PANGEA BM model included age, involved/uninvolved free light chain (FLC) ratio, M spike concentration, creatinine concentration, bone marrow plasma cell percentage (BMPC%), and the haemoglobin trajectory variable. The non-BM model included age, FLC ratio, haemoglobin trajectory, and M spike and creatinine concentration).
Both models were compared to the current criteria (International Myeloma Working Group [IMWG] MGUS and 20/2/20 SMM risk criteria). The C-statistic metric was used to compare the models, in which a C-statistic of 0.5 indicates that the model performs no better than random chance and a C-statistic of 1 indicates perfect prediction. These comparisons were performed during several visits to the clinic.
The PANGEA BM and non-BM models improved the prediction of a progression from SMM to MM compared with the 20/2/20 model. In the PANGEA BM model, the C-statistics increase from 0.533 to 0.756 at patient visit 1 to the clinic, 0.613 to 0.720 at visit 2, and 0.637 to 0.756 at visit three in validation cohort 1. In the PANGEA non-BM model, the C-statistics increase from 0.534 to 0.692 at visit 1, 0.573 to 0.693 at visit 2, and 0.560 to 0.692 at visit 3 in validation cohort 1. The PANGEA models also improved the prediction for a progression of MGUS to MM over the classic IMWG rolling model at visit 1 in the validation cohort 2, with C-statistics increases from 0.640 to 0.729 for the PANGEA model (BM) and 0.670 to 0.879 for the PANGEA non-BM model.
The study findings suggest that both PANGEA models outperform the current criteria in predicting the risk of progression to MM. The use of the PANGEA models in clinical practice will allow patients with precursor disease to receive more accurate measures of their risk of progression to MM, thus prompting more appropriate treatment strategies.
Reference